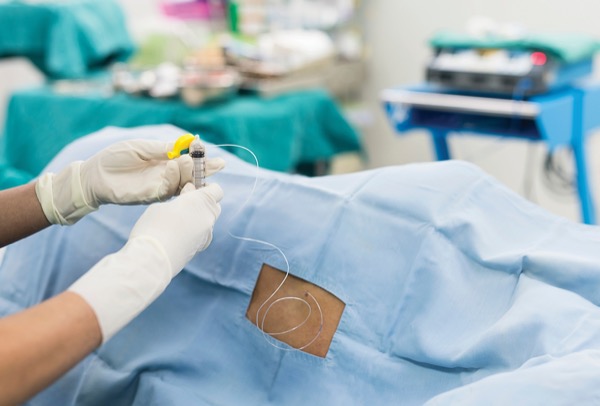
SAN DIEGO—Anesthesiologists play a key role in preventing infectious complications associated with regional anesthesia and pain management.
To clarify the specifics of this role and highlight particular areas of concern, the ASRA Pain Medicine Infection Control Guidelines Committee has been working to develop evidence-based guidelines for best practices for infection control, which will be published soon in Regional Anesthesiology and Acute Pain Medicine.
“This is a very bread-and-butter topic because we do a lot of neuraxial blocks, peripheral nerve blocks and catheters to help with pain relief,” said Hari K. Kalagara, MBBS, MD, an assistant professor of anesthesiology and perioperative medicine at Mayo Clinic in Florida, Jacksonville. “We want to lead with available best clinical practice guidelines across the country in order to prevent infections while conducting regional anesthesia.
“We’re focused on two main things: How do you practice and how do you ensure that the things you are practicing are safe in order to prevent infections?” he said. “Everyone has different approaches—the ER, ICU and anesthesia. We want to get everyone onto the same page and develop best-practice guidelines to keep all patients safe.”
Among key infection risks is catheter colonization, which the workgroup found to be common and related to catheter duration of more than four days. Peripheral nerve block catheters have a greater incidence of colonization than neuraxial catheters, and the risk for infection increases with prolonged use.
Among many other topics related to how anesthesiologists can minimize infection risk, the guidelines focus on the importance of hand hygiene and sterility; perioperatively optimizing blood glucose levels; and dealing with specific medical comorbidities, such as diabetes, obesity, malnutrition and cancer, which are associated with increased risk for infection. Special emphasis is given to the handling of ultrasound transducers or probes, ultrasound gel, and probe covers.
While Kalagara and his colleagues noted the ambitious task involved in creating guidelines for such broad, and often understudied topics, they hope their findings will serve as a blueprint to guide clinical care and clinical decision making for those looking to prevent surgical site infections while conducting regional anesthesia.
The aim is that the guidelines will act as a living document, with regular updates to reflect the evolving state of the field.
By Ethan Covey
Kalagara reported no relevant financial disclosures.