At the 2023 annual meeting of the Society of American Gastrointestinal and Endoscopic Surgeons, researchers from around the world offered the latest in surgical technology—with the potential to transform surgical practice.
Here, OR Management News presents an overview of three devices described during SAGES’s emerging technology session.
First Reported Series of Hugo in General Surgery
Surgeons from Israel reported that they performed 20 consecutive general surgery cases successfully with the Hugo robotic-assisted surgery platform.
The operations included inguinal hernia repair (seven), incisional hernia repair (two), Heller myotomy (three), esophagectomy (two), diaphragmatic hernia repair (one), one-anastomosis gastric bypass (three) and colectomy (two).
The procedures were carried out by three surgical teams at one hospital.
In November 2022, Gadi Marom, MD, was part of a surgical team from Hadassah University Medical Center, in Jerusalem, that performed the first general surgery case using Hugo in Europe, the Middle East and Africa.
The operation was an inguinal hernia repair, a relatively simple case that “helped us build our confidence and dexterity,” said Dr. Marom, a surgeon at Hadassah Hebrew University Medical Center. After the first case, they expanded their practice to use Hugo in different general surgery procedures.
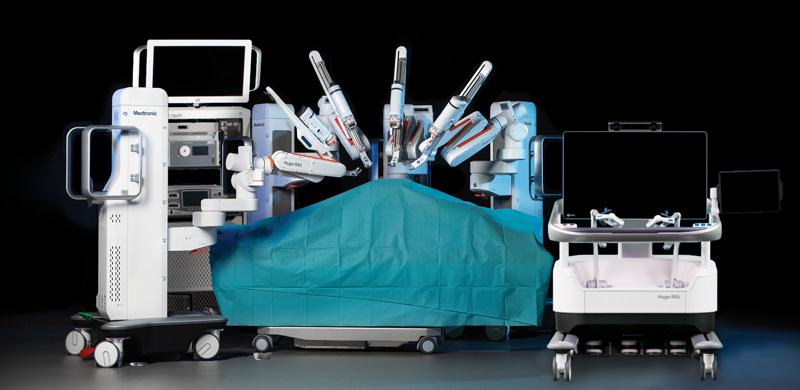
The Hugo system is made by Medtronic and consists of up to four separate carts, each with an independent arm. The arms are controlled by a surgeon seated at a console who manipulates the arms through “pistol-like” hand controllers. The carts can be moved around the OR to suit the space, procedure and patient needs.
“We believe that with time and further development of instruments, the independent arms will surpass the standard for robotic design,” Dr. Marom said.
The system combines wristed instruments, 3D visualization, and a cloud-based surgical video capture option in Touch Surgery Enterprise with dedicated support teams specializing in robotics program optimization, service and training.
In the United States, the system is an investigational device and is not for sale. In October 2022, it received a license from Health Canada for a general laparoscopic surgery indication and it is CE marked in the European Union.
This spring, there were several published reports of Hugo used in general surgery procedures. Italian surgeons described three robotic-assisted colectomies, with mean docking and console times of eight and 259 minutes, respectively (Updates Surg 2023;75[3]:775-780). In Spain, surgeons described a robot-assisted fundoplication for hiatal hernia (Int J Surg Case Rep 2023;106:108178). The operative time was 97 minutes and docking time three minutes.
Success in First Clinical Trial of Magnetic-Assisted Robotic Surgery
There were 46 patients who underwent successful general surgery procedures with magnetic-assisted robotic surgery (MARS) in the first clinical trial of this novel approach, surgeons reported.
This innovation combines magnetic surgery—which is designed to reduce the number of trocars needed for laparoscopic surgery—and robotic surgery.
The system consists of two robotic arms that control an external magnetic controller and a laparoscopic camera. From outside the patient’s body, the magnetic controller allows a surgeon to transabdominally manipulate an internal grasper. The second arm gives the surgeon control of a laparoscopic camera with a stable view.
With MARS, the surgeon stands next to the patient in the sterile field. This is different from other robotic platforms.
For this study, surgeons used MARS to perform cholecystectomy (15 cases), bariatric surgery (16), radical/total and partial nephrectomies (12) and adrenalectomy (three).
The procedure times were 64 minutes for cholecystectomy, 66 minutes for sleeve gastrectomy, 198 minutes for radical/total/partial nephrectomy and 136 minutes for adrenalectomy.
All cases were performed with one fewer trocar than required for traditional laparoscopic or robotic surgery, and there were no complications or serious side effects. All patients were discharged in the first 24 hours and had uneventful follow-up visits at seven and 30 days after surgery.
“At the very least, I think this demonstrates the feasibility of a combination of two technologies of magnetics and robotics, and there may be new opportunities to combine these technologies to provide less invasive approaches to our patients,” said Matthew Kroh, MD, the vice chair of innovation and technology at Cleveland Clinic, and a professor of surgery at Cleveland Clinic Lerner College of Medicine, in Ohio.
The system is small and portable, making it a good fit for an outpatient or ambulatory surgery center, he added.
The first 30 cases of this series were reported in the Annals of Surgery (Open) last winter (2022;3[4]:e225).
The patients were 22 females and eight males, with a mean age of 39 years (range, 22-69 years) and a median body mass index of 33kg/m2 (range, 21.6-50.4kg/m2).
No device-related serious adverse events were reported. However, there were two minor adverse events related to the device: a minor liver abrasion and abdominal wall petechiae. Both resolved without any clinical symptoms or sequelae.
“The combination of magnetic surgery plus robotics may provide benefit to both patients and surgeons. This novel emerging technology should undergo additional evaluation in a more generalized setting for further analysis and broader applications,” the authors concluded.
The MARS procedures were performed with the Levita Robotic Platform. As an investigational system, it is not available for commercial sale in the United States and has not been cleared by the FDA.
Automated Laparoscopic Camera Washer Available in the U.S.
The first automated camera washer for minimally invasive surgery—the troCarWash from Bayou Surgical—is available now in Texas and is expected to be released soon across the United States.
The device received 510(k) clearance from the FDA this February.
Surgeons from Baylor College of Medicine invented troCarWash so that they could clean a laparoscopic camera lens without having to remove it from the operative field during surgery.
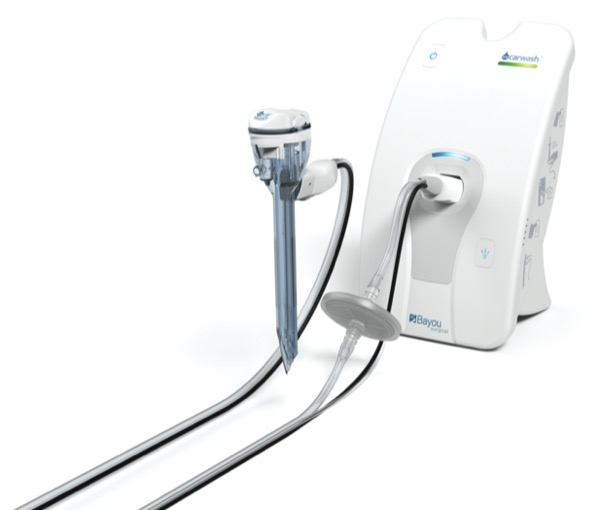
The troCarWash system consists of a standard port with an optical sensor at the distal end that delivers a burst of saline-based cleaning solution, which is aerosolized by the carbon dioxide insufflation, on the camera lens after the camera is pulled slightly back into the port.
Each time the sensor detects the presence of the camera in the port, the wash system is triggered.
“The trocar wash cleans without removing the camera from the operative field, without additions to the scope and with minimal user interaction with the system,” said Bryan Burt, MD, a professor and the chief of thoracic surgery at Baylor College of Medicine, in Houston.
At SAGES, Dr. Burt presented results from in vivo testing of troCarWash in an animal model. Assessors studied images taken by the camera, evaluating image clarity and cleaning efficacy. Results showed a significant (P<0.01) increase in pixel values after washing the laparoscopic camera.
Past studies showed that surgeons spend significant amounts of time cleaning the camera during a laparoscopic operation. In one observational study of 25 procedures amounting to 64 hours of laparoscopy, surgeons had impaired vision 37% of the time due to a soiled lens (Surg Laparosc Endosc Percutan Tech 2016;26[4]:286-289). Overall, 7% of operative time was used in cleaning the distal lens.
The troCarWash was developed through a partnership with Biotex and a collaboration with the Center for Device Innovation, a Johnson & Johnson facility.