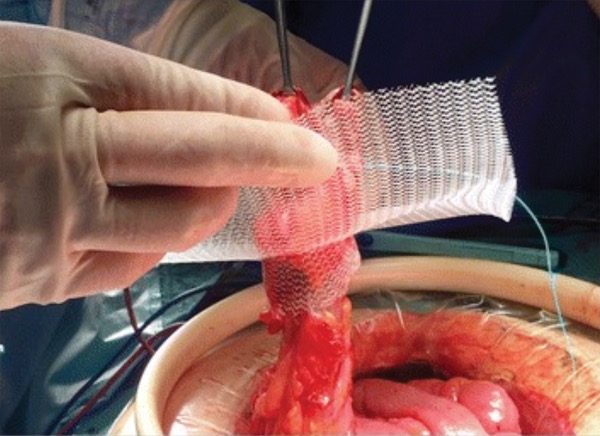
Patients who received synthetic mesh, which costs about 0.5% of a similarly sized piece of biologic mesh, had comparable outcomes after parastomal hernia repair to patients who received biologic mesh, according to a post hoc analysis of a multicenter randomized trial (J Am Coll Surg 2022;235[3]:401-409).
The analysis showed that, among 108 patients included in the trial who underwent open parastomal hernia repair, there were no differences in wound morbidity, reoperations, two-year recurrence rates or quality of life (QOL) based on mesh type.
“Our results indicate that biologic and synthetic mesh have similar safety profiles for retromuscular parastomal hernia repair,” wrote the researchers, who are leaders in hernia surgery in the United States, hailing from five large referral centers for abdominal core health and hernia repair.
But the study also highlights the challenges of open parastomal hernia repair as it is currently performed in the United States. Wound morbidity rates were high, despite investigators’ significant experience and skill. In total, 29.6% of patients experienced a surgical site occurrence that required a procedural intervention, and close to 30% developed a parastomal hernia recurrence within two years of surgery.
“We have a long way to go to make that operation better,” said lead author Michael Rosen, MD, a professor of surgery and the medical director at the Cleveland Clinic’s Comprehensive Hernia Center. “It didn’t really matter what the mesh was—it didn’t perform great.”
Given the potential for complications and recurrences, Dr. Rosen said parastomal hernia repair should be performed in patients who are “extremely symptomatic—meaning they can’t wear their bag, they’re having bowel obstructions or daily pain.” When patients are struggling with symptoms, they should be referred to surgeons who regularly perform these repairs, he said.
Patients who underwent hernia repairs in this study (57 received biologic mesh, 51 synthetic mesh) reported significant improvements in QOL, regardless of mesh type.
Ninety percent of patients were followed for at least two years, and 60.2% had radiographic follow-up.
Approximately half had a previous parastomal hernia repair, and around 90% underwent a concomitant midline incisional hernia repair.
Now, the most important question to be answered regarding parastomal hernia repair is not about mesh type but mesh configuration, the researchers said.
In this study, configuration was left to the discretion of the operating surgeon. In total, 79 patients underwent keyhole configuration repairs and 28 received retromuscular Sugarbaker configuration, a technique first described in 2016 by Eric Pauli, MD, the David L. Nahrwold Professor of Surgery at Penn State Hershey Medical Center (Hernia 2016;20[4]:547-552).
Four patients, all of whom had a keyhole repair, had mesh erosion—including two with biologic mesh and two with synthetic mesh.
Dr. Rosen called the pattern a “signal” at this point, but nothing more. However, he and his colleagues are conducting a prospective randomized controlled trial of 150 patients, over an inclusion period of two years, to compare retromuscular keyhole with Sugarbaker mesh configurations.
To date, there is not enough evidence to encourage greater use of the retromuscular Sugarbaker approach, Dr. Rosen said. This approach has promise, but follow-up data are only short term.
Moreover, it is technically challenging and not without risk. In 2017, Dr. Rosen and his colleagues described their early experience with the retromuscular Sugarbaker approach, in which three in 38 patients experienced mesh erosion into the bowel, leading to stoma necrosis, bowel obstruction and/or perforation (Hernia 2017;21[6]:941-949). The patients were not enrolled in the recent study.
However, Dr. Rosen said these “discouraging early results” appear to be related to the transfascial sutures for lateral mesh fixation that surgeons used early on in their experience with this approach. Since eliminating the sutures from their technique, they’ve had fewer mesh-related complications, he said.
Dr. Pauli, a pioneer of the modified retromuscular Sugarbaker configuration—sometimes referred to as a Pauli parastomal hernia repair—called the paper in Journal of the American College of Surgeons a “major step forward in the study of the repair of parastomal hernia.” He applauded the investigators for their tenacity, noting that they had to obtain an investigational device exemption for the FDA to carry out the trial.
In an accompanying editorial, he cautioned that the results should not be extrapolated to different mesh types or abdominal wall locations, and pointed out that the surgeons who participated in the trial are experts working at referral centers for complex hernia care.
“Our results (yours and mine) may vary,” Dr. Pauli wrote.
Jeffrey A. Blatnik, MD, an associate professor of surgery at Washington University School of Medicine in St. Louis and the director of the Washington University Hernia Center, said surgeons must consider their own experience and tolerance for risk.
“What level of risk are you as the surgeon comfortable entertaining? Are you comfortable dealing with a potential for a mesh infection, or would you rather deal with a potential for a hernia recurrence?” he said.
Just as importantly, surgeons need to speak with patients to understand their goals, he added.
“Some patients would rather have a higher risk for recurrence and a lower risk for infection, or vice versa. It’s an important conversation that you have to have with patients and their families leading into surgery about what their goals for the operation are, and what different options you have available to you.”
In the United States, more than 90% of parastomal hernias are repaired with mesh. But the presence of an ostomy increases the wound class from clean to clean-contaminated or contaminated. As a result, many surgeons are reluctant to use synthetic mesh in these cases, worrying that the nonabsorbable material may be susceptible to infection and erode into the ostomy.
Dr. Rosen and his colleagues said the results of their study illustrate the need for surgeons to take cost into account when selecting a mesh. Hospital cost with biologic mesh after 30 days was almost three times more than with synthetic mesh ($44,187 vs. $15,975; P<0.001). The median mesh price for a biologic mesh was $23,026 compared with $105 for synthetic mesh.
Dr. Rosen suggested that hernia repair may one day be considered more like orthopedic joint replacement. From the outset, orthopedic surgeons tell patients the implant ultimately must be replaced. He’d like hernia surgeons to do the same.
“There are no apologies. It’s not that you’re a bad surgeon. This is a bad prosthetic. This is how long what we do works. And I think we need to reset expectations,” he said.