By Tom Rosenthal
Originally published by our sister publication Infectious Disease Special Edition
As the public’s mitigation practices against COVID-19 wane, concern is rising that the current flu season now starting across the United States could be severe.
“Flu is unpredictable, so we cannot really predict the severity of flu,” said Carla Black, PhD, MPH, an epidemiologist in the CDC’s Immunization Services Division, during a media briefing. “What we can say, so far, is that we’ve had two mild flu seasons, and this means we might be ripe for a severe season because people are not taking all the [mitigation] measures they took for COVID.”
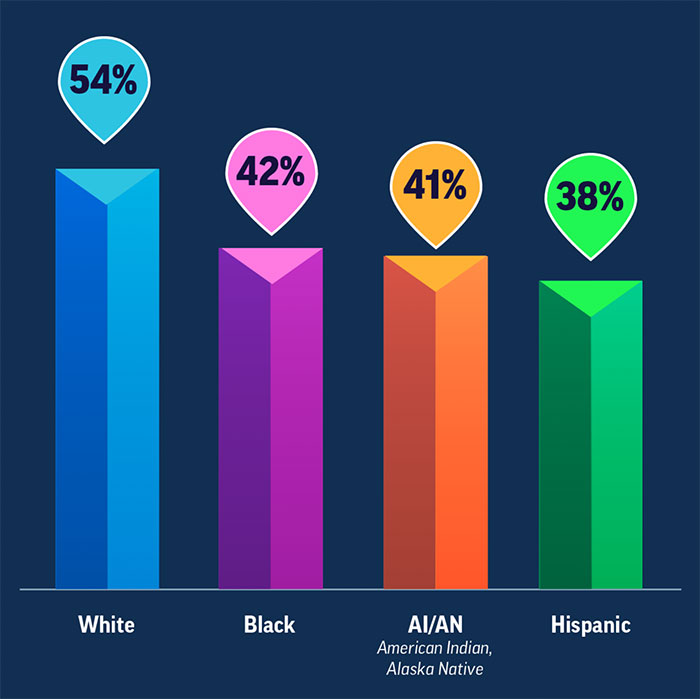 Inequities in flu vaccination coverage continue.
Inequities in flu vaccination coverage continue.Hispanic, AI/AN and Black adults received a flu vaccine at lower rates compared with white adults during the 2021-2022 flu season.
Those two mild seasons might also play a role in the season’s severity. Since there have been fewer cases of flu during the past two seasons, “there’s less natural immunity out there,” Dr. Black said. In addition to shedding their masks and not social distancing, people are increasingly returning to work, traveling again and congregating in public, which also could contribute to a more severe flu season, she said.
“We, of course, want everybody to get vaccinated,” Dr. Black said.
The CDC briefing was for a new Vital Signs report, which found that Black, Hispanic and American Indian/Alaska Native (AI/AN) adults in the United States are more likely to be hospitalized with flu and less likely to be vaccinated against the disease.
The Vital Signs report looked at flu hospitalization rates from 2009 to 2022 and flu vaccination coverage from 2010 to 2022 by race and ethnicity, from two data sources: the Influenza Hospitalization Surveillance Network and Behavioral Risk Factor Surveillance System (MMWR Morbid Mortal Wkly Rep 2022 Oct 18. http://dx.doi.org/10.15585/mmwr.mm7143e1).
“Every year, flu continues to cause severe illness, hospitalization and death,” said CDC acting Principal Deputy Director Debra Houry, MD, MPH. “Unfortunately, flu vaccination rates have been consistently lower among Black, Hispanic and American Indian/Alaska Native adults in the United States since 2010.”
During the 2021-2022 season, influenza vaccination coverage was 54% among white and Asian adults, 42% among Black adults, 38% among Hispanic adults and 41% among AI/AN adults, according to the report.
Black, Hispanic and AI/AN adults were hospitalized with flu at higher rates than white adults during most seasons from 2009 to 2022. Compared with white adults, hospitalization rates were nearly:
- 80% higher among Black adults;
- 30% higher among AI/AN adults; and
- 20% higher among Hispanic adults.
The CDC estimates that between 2010 and 2020, influenza resulted in 9 million to 41 million illnesses, 140,000 to 710,000 hospitalizations and 12,000 to 52,000 deaths annually.
“Vaccination is the best defense we have against the worst outcomes of getting the flu,” Dr. Houry said. “Improving access to and trust in flu vaccines among people is critical to help reduce inequities. “
“For more than a decade, CDC has recommended annual flu vaccination for everyone 6 months and older as the best way to reduce the annual burden of flu,” Dr. Black said. “Still, only about half of Americans get a flu vaccine each year.”
There were many reasons for disparities in vaccine uptake, including lack of access to healthcare and insurance, missed opportunities to vaccinate, and misinformation and distrust, according to Dr. Black. “Racism and prejudice also contribute to these inequities,” she noted.
During the past two years, the CDC launched programs to address barriers to flu vaccination and raise awareness about its importance, specifically among people from racial and ethnic minority groups. They are the Partnering for Vaccine Equity program and a targeted, national flu vaccination campaign. These programs directly led to 1.74 million people receiving either COVID-19 or flu shots, the CDC said.
